How Can We Help?
Why is it important to consider assumptions when we communicate?
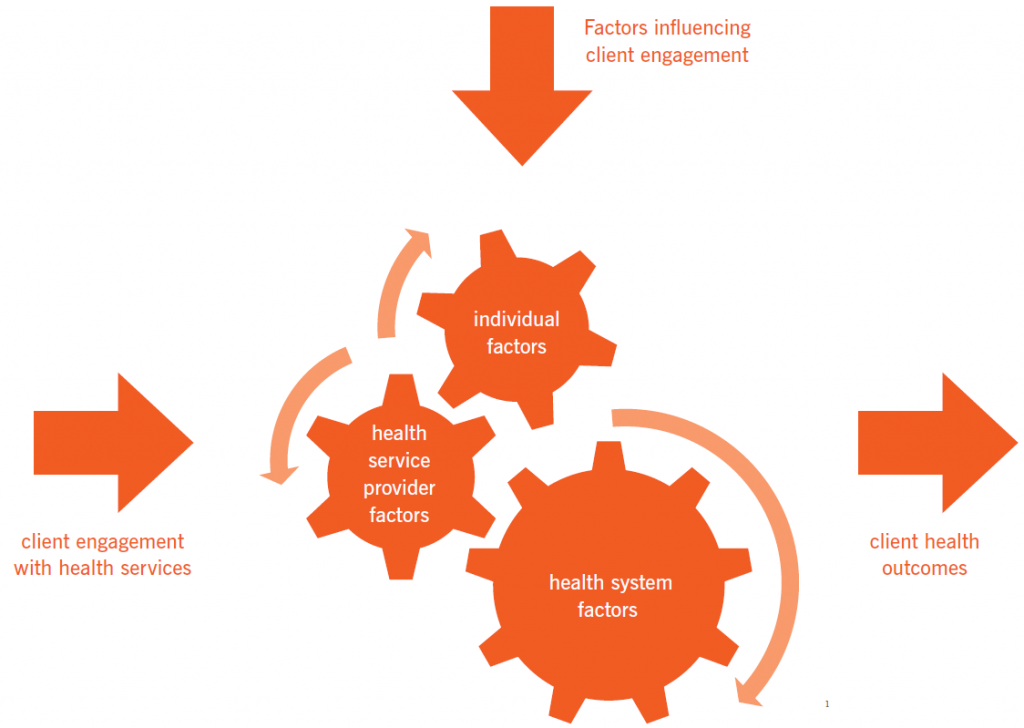
Both clients and health professionals have pre-existing assumptions that they bring with them when they communicate in the health service environment. Assumptions and preconceptions are a result of culture, background and experience. Health outcomes for the client are influenced by these assumptions. Understanding these factors can strengthen communication with clients and improve access, use and engagement with health services.
Individual factors
A number of inter-related client factors impact on the communication encounter. These include:
- The social determinants of health of each client – e.g. socio-economic status; education; religion
- The knowledge a client has – e.g. of the health system, of their illness and how their body works
- The skills a client has – e.g. literacy, numeracy, cognitive
- Cultural beliefs and values
- Experiences that the client has had, particularly past experiences of the health system and the service provider
Service provider factors
Both health professionals and the services they work for also impact on the communication encounter. Some of these factors include:
- The complexity of navigating the health service
- The level of skills of the health professional
- The individual backgrounds and experiences of the health professional
- Time allocated to client interaction by the health professional
- The services’ commitment to client-centred care
- The existence of policies to build the capacity of staff
- Commitment by the service to appropriate communication tools – e.g. teach-back technique, plain language
Health system factors
When looking at health systems overall, key factors play a role in influencing the success of the health professional / client encounter, and contribute to a health literate environment. Included are:
- Federal and State government policies towards health literacy
- Health education as part of the overall education system
- Resources dedicated to a health literate health system
- Policies targeting social determinants of health that impact health literacy
- Focus on community health care versus individual centred models of health
- Support for the most vulnerable clients and communities within the health system
Reference: 1. Adapted from Paasche-Orlow and Wolf, 2007. American Journal of Health Behaviour
English Resource:
![]() Health literacy – assumptions in the communication encounter (PDF)
Health literacy – assumptions in the communication encounter (PDF)
Last reviewed: Dec 2015
Resource Type: Tip/Fact Sheets